Sleep is a vital physiological process with great role for nurses, especially those serving critical care units. However, irregular shifts, high stress, workload, and environmental factors frequently disrupt their sleep. Global studies show that 54.6 to 79.8 percent of nurses experience sleep disturbances, with up to 70 percent affected in some fields. Inadequate sleep impairs decisionmaking, alertness, and patient safety, increasing the risk of medical errors (Segon et al, 2022).
Critical care nursing further intensifies these challenges, often leading to burnout and stress from heavy workloads, unpredictable schedules, interpersonal issues, and personal health concerns. In India, 87.4 percent of nurses report significant stress, which, combined with poor sleep, contributes to depression, anxiety, and reduced job satisfaction. There is evidence of a bidirectional relationship between stress and sleep quality, where each worsens the other. The widespread poor sleep quality and elevated stress levels among nurses are pressing issues that healthcare systems must address. Effective interventions, such as promoting sleep hygiene, implementing stress management strategies, and adopting flexible scheduling can help alleviate these challenges (Mohite et al, 2014).
Need for the study:Poor sleep and high stress among critical care nurses negatively affect health, performance, and patient safety. Irregular shifts, workload, and emotional strain lead to fatigue and impaired concentration, while unclear roles and interpersonal conflicts increase stress. These factors create a cycle where stress and poor sleep worsen each other. Addressing these challenges through sleep hygiene practices, stress management, flexible scheduling, and adequate staffing is essential to safeguar both nurses’ wellbeing and patient outcomes.
Objectives
This study sought to:
Assess the (a) quality of sleep and (b) perceived stress among Nursing Officers working in critical care units of Govt Medical College & Hospital (GMCH), Chandigarh;
- Find the association of (a) quality of sleep with perceived stress and (b) socio-demographic variables with quality of sleep and perceived stress;
- Develop an information booklet regarding the promotion of sleep hygiene and effective coping strategies against stress.
Review of Literature
Many studies highlight poor sleep quality among healthcare professionals. A study of 605 nurses reported poor sleep linked with fatigue and decision regret (Tsegay et al, 2023), while a 2022 multicentre study of 421 clinicians found 81.5 percent had poor sleep aggravated by night shifts (Saberi et al, 2020). Similar findings were reported Natekar et al (2022) in ICU nurses (61.7% poor sleep) among 100 nurses, where marital status and work experience influenced sleep quality (Petrosino et al, 2024). A 2023 cross-sectional analysis confirmed persistent poor sleep and emotional exhaustion among critical care nurses (Masa'Deh et al, 2017).
A comparative study in Jordan hospitals reported the greatest stress in psychiatric, oncology, ICU, and emergency units, while during COVID-19, Indian medical students and doctors, especially postgraduates and residents, showed elevated stress related to education, family health, and unsafe work environments (Agrawal et al, 2021; Rocha & Martino, 2010).
The association between poor sleep and stress is well established. A 2010 study of 203 nurses reported medium stress and poor sleep (PSQI 6.8) (Ravi et al, 2021). During COVID-19, over 60 percent of healthcare workers reported sleep disturbances and over 50 percent moderate-tohigh stress, with a significant positive correlation (r = 0.512, p < 0.001) (Amin et al, 2023). Similar findings were noted in medical students, where 69 percent had moderate stress with a strong PSSPSQI association (p = 0.001) (Zhou Y et al, 2023). A large study of 2,780 nurses confirmed that moderate-to-severe sleep problems with high stress increased risk of depressive symptoms (Sandamali et al, 2024).
Research hypothesis: There is a statistically significant association between the quality of sleep and perceived stress among Nursing Officers working in critical care units. It further assumes that selected socio-demographic variables such as age, education, work experience, and area of posting are significantly associated with both sleep quality and perceived stress at a p < 0.05 level of significance.
Methodology
This descriptive study was conducted from May 2024 to June 2024 to assess sleep quality and perceived stress among 85 Nursing Officers working in critical care units in GMC&H, Chandigarh.
Sample size: 85 Nursing Officers from critical care units were included in the study. The sample size was calculated based on the anticipated 67 percent of nursing officers who reported poor quality of sleep. In an earlier study assuming a 95 percent confidence interval and 10 percent permissible error, the sample size was calculated using the Cochran formula (Zhou et al, 2023).
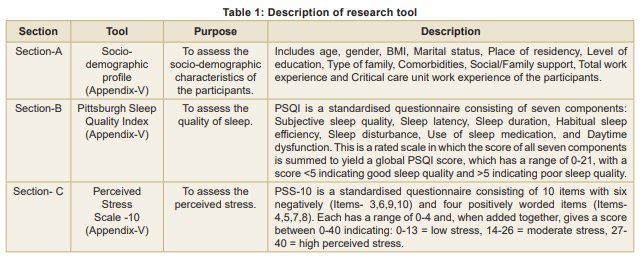
Tools used: The research utilised standardised tools (Table 1), including the Pittsburgh Sleep Quality Index (PSQI) and the Perceived Stress Scale-10 (PSS-10), along with socio-demographic characteristics (Table 2). The PSQI demonstrated high reliability (Cronbach’s α = 0.83) (Lee et al, 2012), and the PSS-10 showed consistent reliability (Cronbach’s α > 0.7) (Kumar S et al, 2021).
Ethical consideration & data collection: This descriptive study was conducted from May-June 2024 among 85 Nursing Officers from critical care units of GMCH Chandigarh, selected through simple random sampling. Standardised tools (PSQI and PSS-10) and a socio-demographic profile were used. Ethical approval was obtained from the Research and Ethical Committee. Informed consent was taken. Data were analysed using SPSS version 20, and descriptive statistics to summarise the data and inferential analysis, i.e. Pearson correlation, to explore relationships between variables.
Results
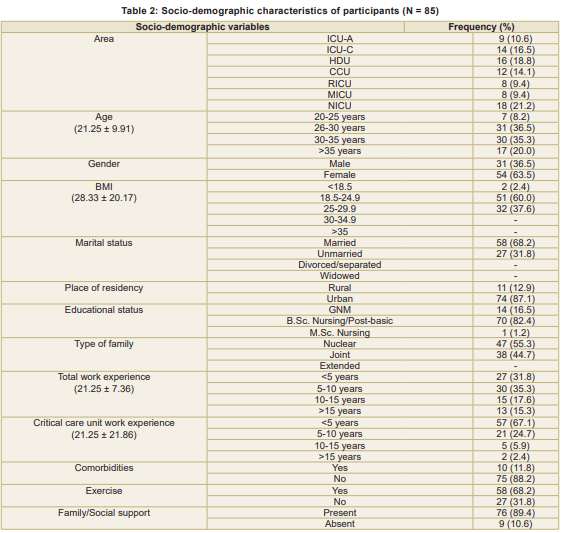
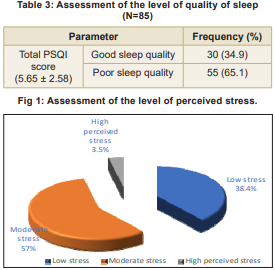
This study assessed sleep quality and perceived stress of the participants using the PSQI and PSS-10. Socio-demographic characteristics of participants is in Table 2. It was found that 65.1 percent of participants had poor sleep quality, while 34.9 percent reported good sleep (Table 3). Among 85 participants, 38.4 percent experienced low stress, 57.0 percent moderate stress, and 3.5 percent high stress, suggesting that most participants managed stress effectively (Fig 1).
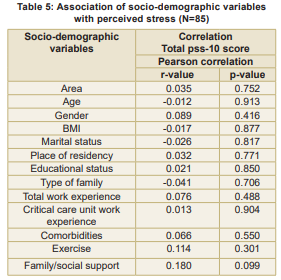
Socio-demographic factors showed weak and statistically insignificant associations with sleep quality, except for a moderate negative correlation between the area of work and quality of sleep (p < 0.001), and weak positive correlations with education level (p = 0.034). Moreover, there was a negative correlation between total work experience (p = 0.045) and critical care work experience (p = 0.008) (Table 3).
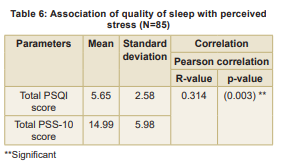
Similarly, perceived stress showed no significant associations with socio-demographic factors such as age, gender, BMI, marital status, work experience or family support (p > 0.05). Mean scores for PSQI and PSS-10 were 5.65 (SD =2.59) and 14.99 (SD = 5.99), respectively. A moderate positive correlation was found between perceived stress and sleep quality (r = 0.314, p = 0.003), indicating that higher stress levels are linked to poorer sleep quality. The findings highlight
the need for interventions to manage stress and improve the quality of sleep (Tables 4-6). The findings confirmed the research hypothesis. A significant positive correlation (r = 0.314, p = 0.003) was observed between quality of sleep and perceived stress, indicating that the hypothesis was accepted.
Discussion
Nurses working in critical care units face a high risk of poor sleep due to the demanding and stressful nature of their work, which negatively impacts both their health and the quality of patient care. This study revealed that 65.1 percent of Nursing Officers working in critical care units at GMCH-32 had poor sleep quality and 57.0 percent experienced moderate stress, with only 3.5 percent reporting high stress. These results align with earlier reports of poor sleep (~68%) and moderate stress among critical care nurses and healthcare staff during the COVID-19 pandemic (Amin et al, 2023).
The moderate positive correlation found between perceived stress and sleep quality (r = 0.314, p = 0.003) supports the bidirectional relationship identified in earlier studies, with 78.4 percent reporting poor sleep and 67.1 percent experiencing moderate stress (Amin et al, 2023; Buysse et al, 1989). The present study also found limited associations between socio-demographic factors and perceived stress, but some significant associations with sleep quality, particularly in areas of work, education, and work experience. Nurses in high-intensity areas such as ICUs or emergency wards may be more vulnerable to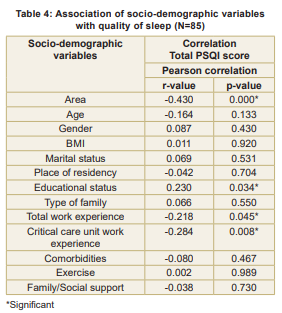
poor sleep, while higher education may improve coping strategies. These findings are broadly in line with earlier reports showing mixed results for demographic predictors of sleep and stress.
The results emphasise the need for interventions targeting both sleep hygiene and stress management. Hospital administrators can support Nursing Officers by implementing flexible scheduling, adequate staffing, and wellness programmes, including yoga, meditation, and counselling. Nurse educators should integrate stress and sleep management into curricula to
prepare future nurses. Such strategies may reduce burnout, improve job satisfaction, and enhance patient safety.
Limitations: The study is limited to Nursing Officers working in critical care units at GMC&H, Chandigarh. There are also potential sample size constraints (N=85).
Implications for Nursing
Nursing practice: Managing stress and sleep enhances nurses’ well-being and patient care.
Nursing education: Integrate stress and sleep management into the nursing curriculum.
Nursing administration: Support staff through wellness programs, including yoga and meditation.
Nursing research: Provides a basis for future studies on stress and sleep in nursing.
Recommendations
- Conduct studies with larger, diverse nursing samples to improve generalisability.
- Implement longitudinal research to assess longterm effects of stress and sleep interventions.
- Explore the applicability of findings among nursing students.
- Evaluate the effectiveness of specific interventions, such as mindfulness meditation, using comparative or experimental designs.
Conclusion
This study evaluated sleep quality and perceived stress among 85 Nursing Officers working in critical care units in GMC&H, Chandigarh. The results revealed poor sleep quality and moderate perceived stress among participants. Socio-demographic factors influenced sleep levels as well. A significant positive correlation (p = 0.003) was found between the quality of sleep and perceived stress, indicating that higher stress levels were associated with poorer sleep quality. These findings highlight the impact of perceived stress on sleep quality among healthcare workers in critical care units, emphasising the need for targetted interventions to improve their well-being.
1. Segon T, Kerebih H, Gashawu F, Tesfaye B, Nakie G, Anbesaw T. Sleep quality and associated factors among nurses working at comprehensive specialised hospitals in Northwest Ethiopia. Front Psychiatry 2022; 13: 931588
2. Mohite N, Shinde M, Gulavani A. Occupational stress among nurses working at selected tertiary care hospitals. Int J Sci Res 2014; 3: 999-1005
3. Shahadan SZ, Ismail MFM, Kamaruzaman KN. Sleep quality and stress levels among nurses: A single-centre study. J Keperawatan Indones 2023; 26(3): 142-52
4. Tsegay Y, Arefayne NR, Fentie DY, Workie MM, Tegegne BA, Berhe YW. Assessment of sleep quality and its factors among clinicians working in critical care units and operating theatres at North West Ethiopia, 2022: A multicenter cross-sectional study. Ann Med Surg (Lond) 2023; 85: 3870-79. doi: 10.1016/j. amsu.2023.10406058
5. Saberi M, Momeni B, Azizi M. The quality of sleep among nurses in critical care units of educational-therapeutic centres of Mazandaran University of Medical Sciences. IJNR 2020; 15(3): 97-109
6. Natekar DS, Dhandargi U, Palabhanvi A, Biradar M, Doddamani H, Marali A, et al. A study to assess the quality of sleep among nurses working in tertiary care hospitals. Int J Sci Healthcare Res 2022; 7(4): 278-81
7. Petrosino F, Bartoli D, Trotta F, Di Nome S, Di Sarli MG, Frammartino R, et al. Nurses' quality of life, sleep disturbance, and intention to leave critical care units: A cross-sectional moderated mediation analysis. Intensive Crit Care Nurs 2024; 81: 103602
8. Masa'Deh R, Alhalaiqa F, Ruz M, Al Dweik G, Akash H. Perceived stress in nurses: A comparative study. Glob J Health Sci 2017; 9(6): 195-203
9. Agrawal N, Sharma H, Dabas A, Mishra A. Perceived stress among medical students and doctors in India during COVID-19 pandemic. MAMC J Med Sci 2021; 7(1): 14-20
10. Rocha MCP da, Martino MMFD. Stress and sleep quality of nurses working different hospital shifts. Rev Esc Enferm USP 2010; 44: 280-86
11. Ravi D, Nagari N, Bobdey S, Yadav AK, Kumar S, Anand V. Perceived stress and quality of sleep among healthcare staff working in a dedicated COVID hospital. J Mar Med Soc 2021; 20 (20): 1-6
12. Amin Y, Mushtaq S, Taj R, Sachdev S, Magray MS. Perceived stress and sleep quality among medical students and their relationship with body mass index and body fat: A cross-sectional study. J Clin Diagn Res 2023. doi:10.7860/ jcdr/2023/63254.18603
13. Zhou Y, Wang S, Liu M, Gan G, Qin N, Luo X, et al. The role of sleep quality and perceived stress on depressive symptoms among tertiary hospital nurses: a cross-sectional study. BMC Psychiatry 2023; 23: 416
14. Sandamali PBGE, De Silva SNAN, Madushani DLA, De Silva YAS, Darshika RUS, Sandakumari HHHS, et al. Quality of sleep and perceived stress among nurses during COVID-19 critical illness. Crit Care Innov 2024; 7(1): 12-23
15. Buysse DJ, Reynolds CF, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh sleep quality index: A new instrument for psychiatric practice and research. Psychiatry Res 1989; 28(2): 193-213
16. Lee EH. Review of the psychometric evidence of the Perceived Stress Scale. Asian Nurs Res 2012; 6(4): 121-27
17. Ghorbani A, Momeni M, Yekefallah L, Shahrokhi A. The association between chronotype, sleep quality, and medication errors among critical care nurses. Chronobiol Int 2023; 40(11): 1480- 86
18. Rasheed SM, Bakhsh LS, Alhameedi RS, Mohidin S. Perceived stress among nurses at a tertiary care teaching hospital in Saudi Arabia during the COVID-19 pandemic. Cureus 2024; 16(3): e554319

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.