Critical thinking skills and clinical judgment are essential for final-year BSc nursing students, as they prepare to transition from academic learning to real-world clinical practice. Critical thinking skills encompass a range of abilities, such as effective communication, technical proficiency, problem-solving, and quick decision-making. These skills are not only basic to performing nursing tasks safely and accurately but also crucial in maintaining patient safety, especially in high-stakes situations like emergency care and intensive care (Välimäki et al, 2024) Without these core competencies, nursing graduates may struggle to deliver care that meets the high standards expected in healthcare, potentially impacting patient outcomes and the overall quality of care (Mohamed, 2018).
Clinical judgment is the ability to assess situations, identify priorities, and make decisions based on evidence, patient needs, and ethical considerations. Strong clinical judgment enables nurses to not only recognise early signs of patient deterioration but also to implement timely Leadership training Critical thinking skills and clinical judgment are essential for final-year BSc nursing students, as they prepare to transition from academic learning to real-world clinical practice. Critical thinking skills encompass a range of abilities, such as effective communication, technical proficiency, problem-solving, and quick decision-making. These skills are not only basic to performing nursing tasks safely and accurately but also crucial in maintaining patient safety, especially in high-stakes situations like emergency care and intensive care (Välimäki et al, 2024) Without these core competencies, nursing graduates may struggle to deliver care that meets the high standards expected in healthcare, potentially impacting patient outcomes and the overall quality of care (Mohamed, 2018). Clinical judgment is the ability to assess situations, identify priorities, and make decisions based on evidence, patient needs, and ethical considerations. Strong clinical judgment enables nurses to not only recognise early signs of patient deterioration but also to implement timely interventions. For nursing students, developing this judgment before facing the full pressures of clinical practice is vital. Simulation-based training, case studies, and mentorship in clinical settings allow them to hone these skills in a low-risk environment, building the confidence needed to take on challenging patient care responsibilities (Mohamed, 2018; Chelagat et al, 2021).
Critical thinking skills and clinical judgment also contribute to effective teamwork, a fundamental aspect of nursing. By developing these competencies, nursing students are better prepared to function as integral members of interdisciplinary teams, advocate for patient needs, and contribute to collaborative patient care (Ayaz & Ismail, 2022). For final-year students, mastering these skills is not only a graduation requirement but also a step towards becoming competent, confident, and compassionate nurses.
Need for the study: Traditional nursing education often focuses on theoretical knowledge, and may not fully prepare students for the complex, real-world scenarios they will encounter (Al Anwer et al, 2022). When combined with simulation-based learning, leadership training, provides an interactive and experiential approach that allows students to practice decision-making in high-stakes situations without risking patient safety (Clemett & Raleigh, 2021). The findings could inform educators and curriculum developers about the value of experiential learning in building confidence and competence among future nurses (Chelagat et al, 2021).
Charotar region in Gujarat is predominantly rural area with two medical college hospitals and many 100-150 bed hospitals with hardly 30 to 40 percent occupancy. It has 15+ nursing institutions offering BSc nursing programme, and not all are able to receive the desired training. Healthcare education in rural locations is notoriously lower quality compared to that in metropolitan areas, due to lack of faculty competence, clinical experience, and access to sophisticated training facilities (Sheshadri et al, 2021).
Schram et al (2024) showed that nursing students' ability to think critically, make sound clinical judgements, and make sound decisions is improved via the use of simulation-based learning. Despite institutions meeting the basic standards stipulated by INC and the state nursing council (which have less stringent guidelines about high-fidelity mannequins), high-fidelity simulation centres are few in Charotar due to financial and physical constraints. The potential of scalable, low-cost simulation treatments to close this gap needs to be evaluated. Clinical judgement is found to be enhanced by exposing nursing students to realistic decision-making settings via simulation-based training in remote areas like Charotar (Koukourikos et al, 2021). Simulation may also proficiently impart leadership skills, including team communication, decision-making under duress, and crisis management (Dopelt et al, 2023). Nurses in remote locations typically confront unique problems like lower patient-to-nurse ratios, increased patient complexity, and fewer resources (Saxena & Godfrey, 2023). Nursing institutions in remote regions suffer from faculty shortages, adversely affecting students' clinical training (Tamata & Mohammadnezhad, 2023). Simulation-based training may alleviate this difficulty by enabling students to practice clinical situations or with limited oversight, so guaranteeing that learning persists despite faculty constraints. The insights gained by evaluating the impact of simulation-based leadership training could be help shaping nursing education policies and practices specific to the Charotar region.
Objectives
This study sought to assess the impact of simulationbased leadership training on critical thinking skills and clinical judgement in final year BSc nursing students.
Hypothesis:
H0 - There is no significant impact of simulation-based leadership training on critical thinking skills and clinical judgement on final year BSc nursing students at a significant level of 0.05.
Review of Literature
Tsaloglidou et al (2021) revealed that the implementation of simulation techniques enables students to practice their clinical and decisionmaking skills in their daily work. The protected environment and the sense of security enhance students' self-esteem and confidence. The study concluded that the development of simulation and instructional techniques can significantly help the students to become integrated and successful healthcare professionals.
In a systematic review, Guibert-Lacasa et al (2022) examined the databases of PubMed, CINAHL, PsycINFO, and Cochrane. Following the PRISMA criteria, data extraction, quality evaluation, and narrative synthesis were carried out to better support nurses' clinical leadership in healthcare facilities. It was estimated that theory-based, mixed-format programmes with many components could be the best option.
In a controlled experiment for evaluating the clinical effects of simulation-based leadership training on team leadership and patient care during real trauma resuscitations, 79 2nd year & 3rd year residents were randomised, and 360 resuscitations were analysed. Participants were assigned at random to either a control group that received conventional orientation or an intervention group that received 4-hour leadership training based on simulation. Video recordings of participants performing real trauma resuscitations in terms of for pre-training behaviours, injury severity score, and post-training group differences in leadership behaviours were tested; 60 people finished the research. Leadership actions after training varied significantly across the experimental and control groups. There was a strong correlation between leadership and patient care in all trauma resuscitations. The study found that participants took their newly acquired abilities into the clinical setting, suggesting that leadership training may indirectly improve patient care via enhanced team leadership (Fernandez et al, 2022).
Another research used video evaluations of a subset of nursing students in situations simulating care for patients with Increased Intracranial Pressure (IICP) to ascertain the efficacy of previously developed nursing care simulations. The subjects were senior nursing students from a South Korean university and a mixed-method approach was used. Seeing the experimental group's simulation movies after administering tests to a control group was not identical to the experimental one. There were 38 students in the experimental group and 39 in the control group, divided into nine teams. The experimental group's movie was reviewed directly to assess their anxiety levels, critical thinking abilities, performance, theoretical knowledge, and clinical judgments. The experimental group showed statistically significant improvements in confidence, theoretical understanding, and clinical performance.
After watching the simulation videos, they came up with 10 clinical judgment processes, such as ‘Identify the patient's condition’ and ‘Reassess the condition after symptoms improve’. They concluded that creating a simulation for nursing care helps students improve their clinical judgement, theoretical knowledge and clinical performance.
Alrashidi et al (2023) conducted a literature review to find out whether student nurses' confidence levels are higher during clinical practice after using simulation using suitable key words and Boolean operators. Pertinent studies were extracted from five academic databases: CINAHL, EBSCO, ProQuest, PubMed, and Medline. All studies were published ones during 2005-2020; 15 of these were retrieved for evaluation, and four main points were uncovered: enhanced self-assurance in performing clinical duties, enhanced capacity for teamwork, enhanced selfassurance in carrying out community service, and enhanced self-confidence in interacting with patients and colleagues. It was determined that nursing students' self-confidence in their abilities to carry out clinical duties, make clinical judgements, interact with patients and teammates, and enhance collaboration may be enhanced via the clinical simulation.
Methodology
This research adopted a quantitative approach, utilising a quasi-experimental design with a group pre-test and post-test control group design to examine the impact of simulation-based leadership training on critical thinking skills and clinical judgment among final-year BSc nursing students who met the eligibility criteria. Simulation-based leadership training served as the independent variable, while the dependent variables were the critical thinking skills and clinical judgment demonstrated by these nursing students. The study was set in nursing institutions within Charotar region of Gujarat State, selected through cluster sampling to ensure a diverse representation across the region, after seeking the ethical approval.
Inclusion criteria: Final year consenting BSc nursing students of any age or gender having cleared their previous exams up to the third year of exams.
Exclusion criteria: Final year BSc nursing students not available for data collection.
Sample size: Power analysis method was opted to measure the sample size for a significance level of 0.05. The following formula was used to measure:
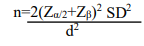
where Zα/2 is critical value for the desired confidence level-1.96 for 95% confidence; Zβ is value for desired power-0.84 for 80% power; SD- standard deviation5; and d- expected effect size-0.5 as medium effect size.
A total of 600 samples were recruited using convenience sampling technique, which were randomly allocated (simple random- computer table method) to both the experimental and control groups, with 300 subjects in each. The data were gathered by using the Critical Thinking Assessment Scale (CTAS) to assess students' critical thinking levels and the Clinical Judgement Assessment Scale (CJAS) to assess the clinical judgement level of nursing students. These tools were validated by 11 nursing educators from medical-surgical, child health nursing and obstetric gynaecological nursing. The reliability of tools was measured and found as 0.89 and 0.84 for CTAS and CJAS, respectively. First, these tools were introduced in the first contact to collect information as a pre-test, then the samples in the experimental group were provided the simulation-based leadership programme for 30 days. Post-test data were collected from both groups on the day 31. The simulation-based leadership programme was broadly scheduled in a 4-week programme. Week 1 - introduction to leadership and critical thinking fundamentals, week 2-covered developing communication and decision-making skills, week 3 covered advanced clinical judgement and critical thinking skills development, week 4 covered leadership practice and programme conclusion. This methodological framework rigorously assessed the effectiveness of simulation-based interventions in enhancing essential competencies in nursing students on the cusp of entering professional practice.
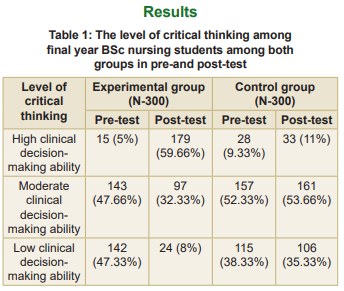
Table 1 revealed that the maximum number of subjects were found in low clinical decision-making ability at the pre-test level. After intervention, in the experimental group, the highest level was found at high clinical decision-making ability, while the control group still found a low level in the post-test level. Table 2 portrays the level of clinical judgement among final year BSc nursing students in both groups in pre- and post-test.
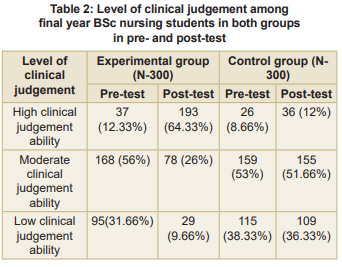
After intervention, in the experimental group, the highest level was found at high clinical judgement ability, while the control group still found a low level in the post-test level.
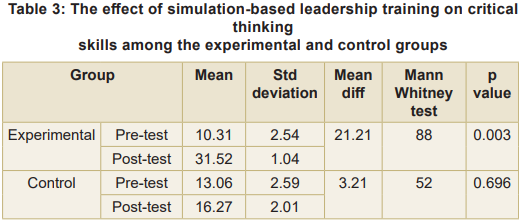
The mean difference between the experimental group was 21.21, and in the control group, it was 3.21 for critical thinking skills among final year BSc nursing students (Table 3). The experimental group calculated p-value was found at 0.003 and effectiveness was found significant. Thus, intervention simulation-based leadership training was found effective, and the null hypothesis H0 was rejected at 0.05 level of significance.
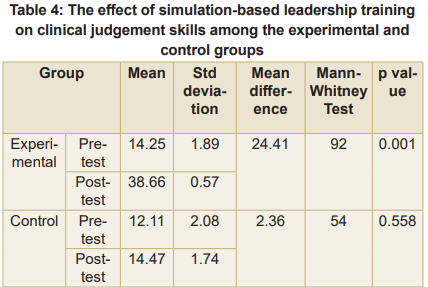
The mean difference between the experimental group was 24.41, and in the control group, 2.36 for clinical judgement skills among final year BSc nursing students (Table 4). The experimental group calculated a p-value as 0.001. A significant effectiveness was found showing that provided intervention simulation-based leadership training was effective and the null hypothesis H0 was rejected at the 0.05 level of significance.
Discussion
The simulation-based leadership training was found to be significantly effective in enhancing the critical thinking and clinical judgement of the final year BSc Nursing students. A review article (Elendu et al, 2024) supported that simulation-based training will play a crucial role in preparing the next generation of healthcare professionals, and its ongoing evolution is driven by technological innovations. Another study with intervention of simulation-based training among novice nurses found that completion of the simulation programme was correlated with enhanced clinical judgment of novice nurses (Kawase et al, 2024). Yet other studies (Alrashidi et al, 2023; Alqarni et al, 2023; Vázquez-Calatayud et al, 2022; Onyango et al, 2021; Misisco et al, 2020) also supported current study findings by stating that the leadership programme had a significant impact on health system performance indicators among health professionals.
Nursing Implications
The present study outcomes assisted the researchers in (a) Enhancing clinical decision-making to more effectively evaluate patient conditions, prioritise therapies, and make prompt judgments, particularly in complicated or emergency scenarios; (b) Enhancing leadership capabilities including team management, communication, delegation, and conflict resolution, in authentic environments; Preparing for rural healthcare challenges; Facilitating evidence-based nursing practices; Enhancing student engagement and learning outcomes.
Our results provide evidence for policymakers and nursing education boards to include more simulation-based instruction in the nursing curriculum, particularly in resource-limited, rural environments.
Recommendations
Future studies should consider expanding the research to nursing students in rural and urban areas across Gujarat, or even at national level, to assess whether the impact of simulation-based leadership training is consistent across different geographical and demographic groups.
- A follow-up study should be conducted at 6 months, 1 year, or longer after the intervention to assess how well the critical thinking and clinical judgment skills gained through simulation are retained.
- Future research may: explore the impact of simulation training on other nursing competencies, like communication skills, teamwork, patient safety, ethical decision-making, and cultural competence; examine the effectiveness of different types of simulation models (e.g., high-fidelity simulation, lowfidelity simulation, virtual simulation, role-playing, and case-based scenarios) on developing critical thinking, leadership, and clinical judgment; etc. to provide a more robust comparison of the effectiveness of simulation-based training versus conventional methods; examine how faculty training and educator experience in simulation-based teaching affect the outcomes of simulation interventions; and consider exploring the psychological preparedness and confidence of nursing students after simulation training, especially in high-stress clinical environments.
Conclusion
The evolution of nursing education necessitates integration of simulation into the curriculum to cultivate a more competent, confident, and adaptive nursing staff. This method enhances individual skills and fortifies the healthcare delivery system by equipping future nurses to tackle the problems of healthcare settings. Additional study with longitudinal follow-up and varied geographic samples, will be essential in assessing the long-term advantages and scalability of simulation-based training in nursing education.
1. Välimäki M, Hu S, Lantta T, Hipp K, Varpula J, Chen J, et al. The impact of evidence-based nursing leadership in healthcare settings: a mixed methods systematic review. BMC Nurs 2024; 23(1): 45
2. doi: 10.1186/s12912-024- 02096-4 2. Mohamed NT. Relationship between leadership styles and clinical decision-making autonomy among critical care nurses. Egypt Nurs J 2018; 15(2): 102-111
3. Michael NA, Chinweike Ikwe, Judith CI. Effectiveness of simulation-based training in medical education: Assessing the impact of simulation-based training on clinical skills acquisition and retention: A systematic review. World J Adv Res Rev 2024; 21(1): 1833-43
4. Chelagat T, Rice J, Onyango J, Kokwaro G. An assessment of the impact of leadership training on health system performance in selected counties in Kenya. Front Public Heal 2021; 8 (Feb): 1-12
5. Ayaz O, Ismail FW. Healthcare simulation: A key to the future of medical education - A review. Adv Med Educ Pract 2022; 13: 301-08
6. Al Anwer AHM, Banakhar MA, Elseesy NAE. Clinical leadership behaviors among critical care nurses in private and governmental hospital: A cross-sectional survey. Int J Nurs Sci 2022; 9(3): 357-63
7. Clemett VJ, Raleigh M. The validity and reliability of clinical judgement and decision-making skills assessment in nursing: A systematic literature review. Nurse Educ Today 2021;102:104885
8. Sheshadri V, Wasserman I, Peters AW, Santhirapala V, Mitra S, Sandler S, et al. Simulation capacity building in rural Indian hospitals: A 1-year follow-up qualitative analysis. BMJ Simul Technol Enhanc Learn 2021; 7(3): 140-45
9. Schram A, Bonne NL, Henriksen TB, Paltved C, Hertel NT, Lindhard MS. Simulation-based team training for healthcare professionals in pediatric departments: Study protocol for a nonrandomized controlled trial. BMC Med Educ [Internet] 2024; 24(1): 607. Available from: https://doi.org/10.1186/ s12909-024-05602-z
10. Koukourikos K, Tsaloglidou A, Kourkouta L, Papathanasiou I V, Iliadis C, Fratzana A, et al. Simulation in clinical nursing education. Acta Inform medica AIM J Soc Med Informatics Bosnia Herzegovina Cas Drus za Med Inform BiH. 2021 Mar; 29(1): 15-20
11. Dopelt K, Shevach I, Vardimon OE, Czabanowska K, De Nooijer J, Otok R, et al. Simulation as a key training method for inculcating public health leadership skills: A mixed methods study. Front Public Heal 2023;11:1202598 12. Saxena SG, Godfrey T. India’s opportunity to address human resource challenges in healthcare. Cureus 2023 Jun; 15(6): e40274
13. Tamata AT, Mohammadnezhad M. A systematic review study on the factors affecting shortage of nursing workforce in the hospitals. Nurs Open 2023 Mar; 10(3): 1247-57
14. Guibert-Lacasa C, Vázquez-Calatayud M. Nurses’ clinical leadership in the hospital setting: A systematic review. J Nurs Manag 2022 May; 30(4): 913-25
15. Fernandez R, Rosenman ED, Olenick J, Misisco A, Brolliar SM, Chipman AK, et al. Simulation-Based Team Leadership Training Improves Team Leadership During Actual Trauma Resuscitations: A Randomized Controlled Trial. Crit Care Med 2020 Jan; 48(1): 73-82
16. Jang AR, Moon JE. The effect of nursing simulation on the clinical judgment of nursing care for patients with increased intracranial pressure (IICP). Iran J Public Health 2021 Oct; 50 (10): 2055-64
17. Alrashidi N, Pasay AE, Alrashedi MS, Alqarni AS, Gonzales F, Bassuni EM, et al. Effects of simulation in improving the selfconfidence of student nurses in clinical practice: A systematic review. BMC Med Educ 2023; 23(1): 815. Available from: https://doi.org/10.1186/s12909-023-04793-1
18. Elendu C, Amaechi DC, Okatta AU, Amaechi EC, Elendu TC, Ezeh CP, et al. The impact of simulation-based training in medical education: A review. Med (United States) 2024; 103 (27): e38813
19. Kawase Y, Takahashi S, Okayasu M, Hirai Y, Matsumoto I. Effectiveness of a Simulation-based education program to improve novice nurses’ clinical judgment skills. Cureus 2024; 16(6): e61685

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.